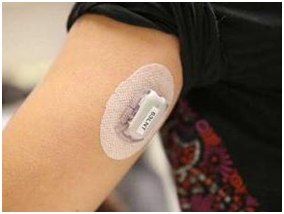
With a blood glucose meter, you use blood to do the test whereas CGM is continuous glucose monitoring.
Continuous glucose monitoring isn’tblood glucose monitoring as the sensor with a CGM device is placed into your body but not into the bloodstream. The sensors measure the glucose in your interstitial fluid -the fluid in and around your body’s cells.
The relationship between glucose concentrations in interstitial fluid (ISF) and blood has generated great interest due to the possibility of gaining up to 288 glucose level readings a day without having to do finger pricks.CGM is less invasive.
Basically, CGMs are a less invasive technique for measuring glucose levels. CGM can be used whether you wear a pump or use injections for your insulin delivery. CGM systems work 24 hours a day and can include alarms to indicate when your glucose levels aretoo high or too low.
Continuous glucose monitoring product guides
Continuous Glucose Monitoring (CGM) is steadily becoming the method of gaining greater control for people on intensive insulin therapy.
HOW DO I ACCESS SUBIDISED CGM ?
AMSL (DEXCOM) PRODUCTS
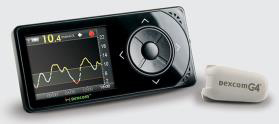
Dexcom G4 Platinum CGM system can be used as a standalone system or with the Animas® Vibe® insulin pump. Here’s how it works:
1. A tiny sensor is placed under the skin in a similar way to an infusion site and is worn up to 7 days at a time. After you have been trained under the supervision of your healthcare professional and AMSL Diabetes representative, you can do this on your own.
2. The Dexcom G4 PLATINUM transmitter is then attached to the sensor.
3. Once the sensor is inserted and the transmitter is attached there is a two hour start-up period where no information will be displayed. After this time, you will need to enter two finger stick readings from your blood glucose meter to calibrate the Dexcom system.
4. The glucose sensor will then continuously measure your interstitial glucose levels (in the fluid space between the cells) and through the transmitter, will send information wirelessly to either your Dexcom Receiver or your Animas® Vibe® insulin pump.
5. After the two initial calibrations, further calibrations are required every 12 hours.
6. Dexcom G4 CGM system guide including VIDEO
7. Product Guide – User Guide, Quick Start, Tutorial

Dexcom G5® Mobile System consists of three components:
1. Small Sensor that measures glucose levels just underneath the skin.
2. Transmitter that is fastened on top of the sensor and sends data wirelessly to your compatible smart device or your receiver.
3. A Display Device which can be a compatible smart device with the Dexcom G5® Mobile app OR the Dexcom G5® Mobile receiver. Either choice of display will show your glucose trends in vivid colours so you can easily see when it’s high, low or within range.
4. Dexcom G5 CGM system guide I Glucose on your phone including VIDEO
5. Product Guide – User Guide, Quick Start, Tutorial
MEDTRONIC PRODUCTS
Medtronic have four products available through the CGM Initiative; the Enlite™ Sensor, Guardian™ 2 Link, MiniLink transmitter, Guardian Connect™ CGM. CGM technology enables a user to monitor glucose levels 24 hours a day through a sensor.
The varieties of Medtronic CGM in Australia
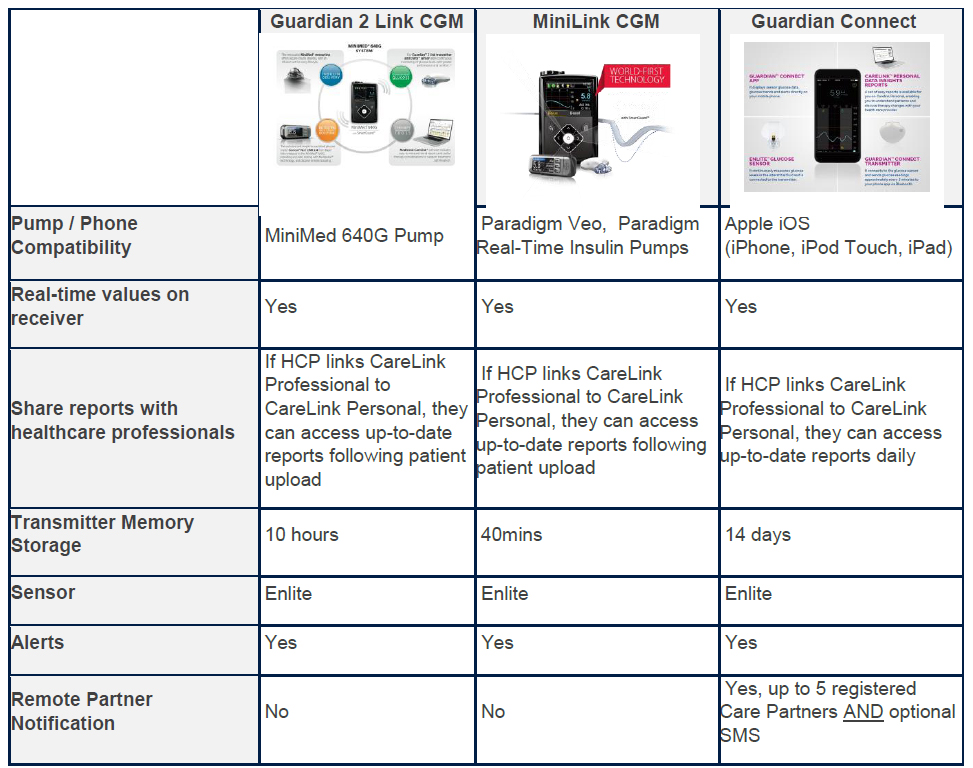
HOW YOU CAN BENEFIT FROM MEDTRONIC CGM
CGM measures and indicates glucose levels continuously [24/7] to assist in monitoring. It can be used by type 1 and type 2 diabetes patients who would like better glucose control to improve the health and quality of their lives – and can help to take the guesswork out of glucose monitoring.
There are two ways you can benefit from Medtronic CGM:
With an insulin pump. With CGM and the Medtronic Veo or MiniMed 640G Insulin Pump, insulin delivery can be automatically stopped to reduce the occurrence or severity of hypoglycaemia. You’ll have the ability to set alerts to warn about highs or lows, and will see the full picture of glucose levels 24/7 on the device.
Without an insulin pump. Guardian™ Connect CGM delivers real-time glucose information direct to your iOS device3. You (and any care partners i.e. family members/carers or healthcare professionals) can be alerted if you’re heading towards hypoglycaemia or hyperglycaemia.
This is important because people who are hypo unaware are six times more likely to have severe hypoglycaemia leading to seizures, coma and even death. Having hypos leads to more hypos and the increased risk of these severe events.
